
Paradigm Case Management
Arcweb Technologies partnered with Paradigm to modernize criminal justice technology with thoughtful design and AI-first justice innovation.
Homestead Smart Health Plans helps self-insured organizations lower healthcare costs through an innovative system of transparent claims adjustment and reference-based repricing technology.
After Homestead identified an opportunity to introduce automation and modern digital systems to the traditionally manual and laborious claims adjustment industry, they partnered with Arcweb Technologies to implement an innovative, cloud-based workflow that helped them grow their business from $2.4 million to over $30 million in revenue.
Self-funded health plans create opportunities for organizations to reduce costs and offer better coverage options for their employees. But the system also creates challenges with claim repricing and reimbursement, a task that has traditionally been handled by specialized vendors using a labor intensive and imprecise system.
Homestead Smart Health Plans saw an opportunity to create competitive advantage by automating its reference-based repricing process. The Arcweb team worked closely with Homestead to transform their methodology using business process automation, modern software, and complex integrations with public data sources used as a benchmark for claims repricing.
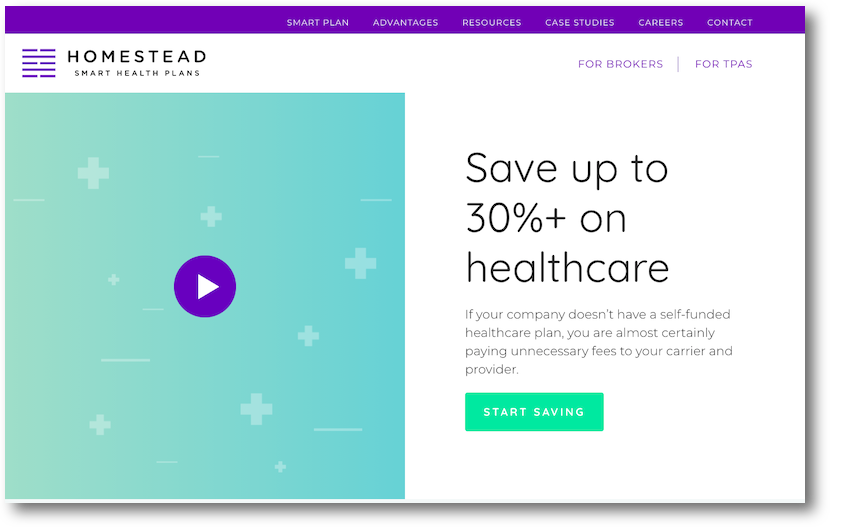
Traditionally, claims repricing relies on a complex paper-based process to deliver accurate information to self-insured and Third-Party Administration (TPA) clients. Homestead wanted to accelerate turnaround and improve efficiency by replacing this system with a modern digital process – they just needed the right partner to bring it to life.
Manual processing and the complex nature of healthcare claims meant that errors and inefficiencies were common in claims repricing. Homestead realized there was a way to save its clients money by eliminating errors and inefficiencies through innovative technology.
Arcweb’s design and engineering teams worked closely with Homestead to plan, design, and execute a digital transformation process for their repricing business.
By working closely with Homestead‘s processing team and claims adjustment SMEs, Arcweb helped Homestead design, build, and launch Claim Watcher, a state-of-the-art repricing tool that uses automation and data integration to accelerate turnaround, reduce inaccuracies, and improve efficiency.
Claim Watcher has helped reduce the health benefits spend of Homestead’s clients by an average of 30%, while allowing Homestead to grow from $2.4 to $30 million in revenue in just a few years.
Digital Transformation
Thanks to the successful launch of Claim Watcher, Homestead has grown to be a leader in the reference-based repricing market. Claim Watcher’s improved efficiency and repricing accuracy has also allowed Homestead to give clients a significant reduction in health benefits spend, along with improved customer satisfaction and a more efficient and accurate claims repricing process.
Market Growth
The Claim Watcher service has also allowed Homestead to work with multiple TPAs, magnifying their impact on the market and helping business owners take a more sustainable approach to the health benefits they can offer their workforce.
By working closely with Homestead‘s processing team and claims adjustment SMEs, Arcweb helped Homestead design, build, and launch Claim Watcher, a state-of-the-art repricing tool that uses automation and data integration to accelerate turnaround, reduce inaccuracies, and improve efficiency.
Claim Watcher has helped reduce the health benefits spend of Homestead’s clients by an average of 30%, while allowing Homestead to grow from $2.4 to $30 million in revenue in just a few years.
Thanks to the successful launch of Claim Watcher, Homestead has grown to be a leader in the reference-based repricing market. Claim Watcher’s improved efficiency and repricing accuracy has also allowed Homestead to give clients a significant reduction in health benefits spend, along with improved customer satisfaction and a more efficient and accurate claims repricing process.
The Claim Watcher service has also allowed Homestead to work with multiple TPAs, magnifying their impact on the market and helping business owners take a more sustainable approach to the health benefits they can offer their workforce.

Arcweb Technologies partnered with Paradigm to modernize criminal justice technology with thoughtful design and AI-first justice innovation.
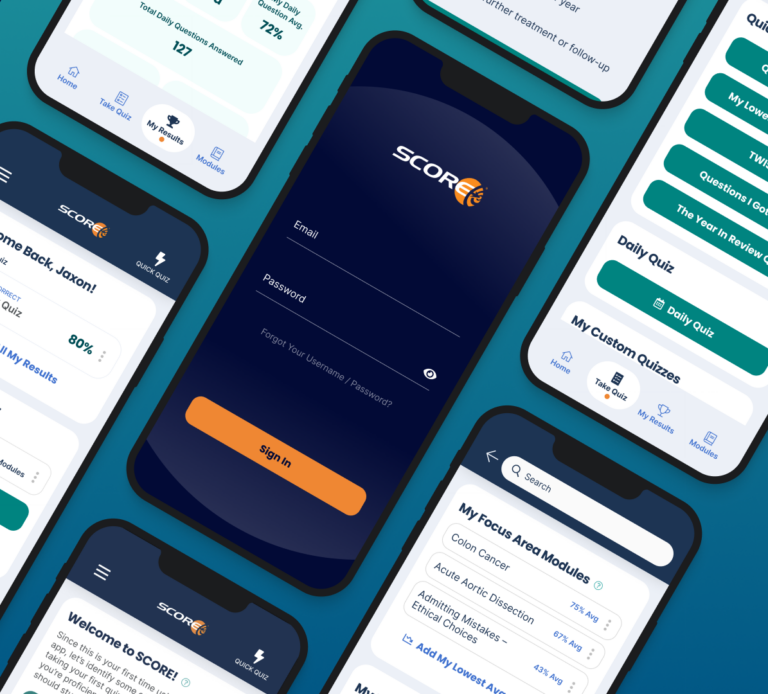
Arcweb developed and executed a strategic go-to-market plan for the American Board of Surgery, enabling an on-time, on-budget launch of a mobile app to make surgical education materials available anytime, anywhere.

Through a combination of product strategy, technology leadership, and software engineering, Arcweb helped Tomorrow Health accelerate the development of critical new functionality for their home-based care ordering platform.